Gynecologic robotic surgery is a relatively new technology that is gaining popularity. One of the most popular gynecological robotic surgeries performed is the robotic-assisted laparoscopic hysterectomy.
While this technology has its advantages, it also has many problems.
Keep reading to learn the differences between robotic and laparoscopic hysterectomy and whether this is the best option for you.
What is gynecological surgery?
Gynecological surgery refers to surgical procedures performed on the female reproductive system. Surgery may be recommended as a treatment for abnormal uterine bleeding, endometrial cancer, fibroids, endometriosis, and uterine or ovarian cancer.
Traditional abdominal surgery (also known as open surgery or a laparotomy) is the most invasive, as it requires cutting open the abdomen. For less invasive options, there is vaginal hysterectomy (removing the uterus through the vagina, requiring smaller incisions). And the least invasive surgical techniques are laparoscopic and robot-assisted surgery.
The best technique varies from patient to patient, but at the Outpatient Hysterectomy Center, we focus on laparoscopic surgeries that treat our patients with the least pain possible.
Common gynecological surgeries include:
- Abdominal Hysterectomy: The surgical removal of the uterus — and sometimes the cervix and other reproductive organs.
- Oophorectomy: The surgical removal of one or both ovaries.
- Tubal ligation: A permanent form of birth control where the fallopian tubes are surgically cut or blocked.
- Myomectomy: The surgical removal of uterine fibroids, which are noncancerous growths in the uterus.
- Endometrial ablation: A procedure where the lining of the uterus is surgically removed or destroyed to treat endometriosis and heavy menstrual bleeding.
- Pelvic organ prolapse surgery: A procedure to repair weakened or damaged pelvic floor muscles that may result in organs such as the uterus, bladder, or rectum bulging into the vaginal canal.
What is robotic surgery?
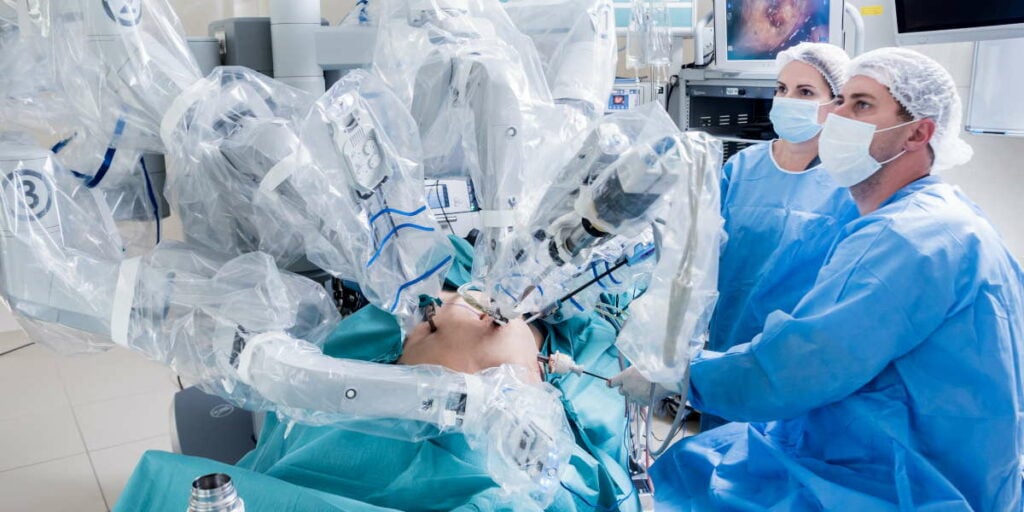
Robotic surgery is a form of minimally invasive surgery that (as the name implies) involves the use of robotic arms and instruments.
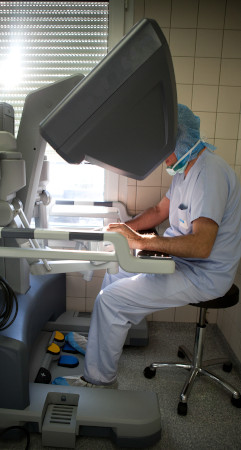
Amongst the most famous surgical system designs is the Da Vinci robotic surgery, when the surgeon uses hand and foot controls to manipulate the robotic arms, which are equipped with tiny instruments and a camera.
The surgeon makes small incisions in the patient’s body and inserts the robotic arms and instruments. The camera provides a magnified, 3D view of the surgical site, which provides better visualization of surrounding tissues.
Robotic surgery pros and cons
Some of the advantages of robotic surgery include:
- less pain
- less blood loss
- smaller incisions
- shorter hospital stays
- quicker recovery times
- better ergonomics for the surgeon
At least one study also suggests that robotic surgery provides better outcomes for obese patients. Patients with a body mass index (BMI) of 30 or higher experienced less blood loss with robotic-assisted laparoscopy than with traditional laparoscopy.
However, robotic surgery also has some disadvantages. These include:
- limited OB/GYN surgeon feedback
- more expensive
- not widely available
- longer operative time
The choice of surgical technique depends on the specific condition being treated and the preferences of the surgeon and patient.

Call 877-760-3564 or click here to schedule online
What is a laparoscopic hysterectomy?
A laparoscopic hysterectomy is a minimally invasive gynecologic surgery that involves the removal of the uterus using a laparoscope — a thin, flexible tube with a camera and light at the end.
The laparoscope is inserted through small incisions in the abdomen, allowing the surgeon to view the surgical site on a video monitor.
The uterus is then detached from the ligaments and blood vessels that hold it in place and removed through one of the incisions.
Here at the Outpatient Hysterectomy Center, we perform laparoscopic hysterectomies because they are less invasive and have less scarring and quicker recovery times.
How does a robotic-assisted laparoscopic hysterectomy work?
A robotic-assisted laparoscopic hysterectomy is pretty similar to a manual one. The main difference is that the instruments are controlled by robotic arms rather than directly handled by the surgeon.
The robotic arm allows for more precise movements and greater dexterity than conventional laparoscopic hysterectomy.
So, is it better to get robotic surgery?
Robotic technology is designed to perform precise surgical procedures in small and delicate spaces. While it can be beneficial in certain surgeries, such as those that require intricate maneuvers, it may not be necessary for all procedures.
A minimally invasive hysterectomy, for example, involves clamping the blood vessels leading to the uterus and surgically removing it. Therefore, there isn’t as much benefit to using a robotic laparoscopy as there might be in other surgeries.
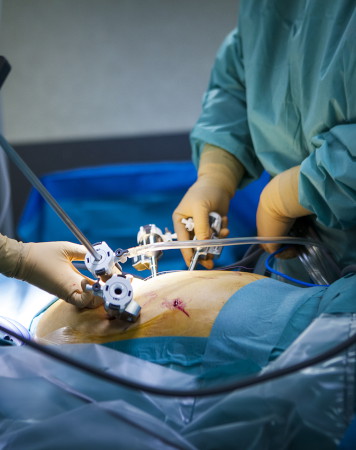
Robotic vs. laparoscopic surgery
Laparoscopic surgery and robotic surgery are both minimally invasive approaches that use specialized instruments to perform surgical procedures.
Multiple clinical and systematic review studies have compared a robotic vs. laparoscopic hysterectomy. However, the studies have been limited and most were retrospective (looking at existing data rather than performing their own studies).
In general, results showed very similar surgical outcomes and complication rates.
Key takeaways: Problems with robotic surgery
Here are some of the problems that patients should be aware of when considering a robotic surgical approach:
- cost
- lack of long-term data
- limited training opportunities
- technical issues
- limited accessibility
- overuse
- steep learning curve
The final word on robotic-assisted gynecological surgery
While there is some evidence that gynecologic robotic surgery can be safe and effective, there is still a lack of long-term data on its outcomes. As such, it is difficult to determine the risks and benefits of the procedure compared to other surgical options.
There are also limited opportunities for surgeons in the department of obstetrics and gynecology to receive proper training in gynecologic robotic surgery. This can lead to a lack of expertise in this area, increasing the risk of complications in comparison to a laparoscopic hysterectomy.
Because reporting of perioperative and postoperative complications is voluntary, the American College of Obstetricians and Gynecologists (ACOG) warns that true complication rates remain unknown.
The most often reported adverse reactions included a slower recovery from anesthesia and an increased likelihood of post-operative complications such as pneumonia, urinary tract infections, abnormal uterine bleeding, and blood clots.
It is essential for patients and healthcare providers to carefully weigh the risks and benefits of this procedure before deciding to use it. Additionally, efforts should be made to improve access to training and ensure that the technology is used appropriately.
At this point, robot-assisted surgery is not consistently superior to human performance in the operating room, especially regarding specific gynecology procedures where there’s no clear-cut benefit to using robotic assistance.
Why choose the Outpatient Hysterectomy Center for your gynecological surgery?
Drs. Aliabadi and Yera are renowned gynecological surgeons. Patients travel from around the country to be treated at the Outpatient Hysterectomy Center and Dr. Aliabadi even travels to teach her surgical expertise to other doctors.
Whether it’s your first consultation or your fifth follow-up, we provide our patients with the same level of attention and care.
We invite you to establish care with the Outpatient Hysterectomy Center. Please make your appointment online or call us at (844) 863-6700.
The Outpatient Hysterectomy Center is conveniently located to patients residing throughout Southern California and the Los Angeles area. At the Cedars-Sinai Medical Center, we are near Beverly Hills, West Hollywood, Santa Monica, West Los Angeles, Culver City, Hollywood, Venice, Marina del Rey, Malibu, Manhattan Beach, and Downtown Los Angeles, to name a few.
Call 877-760-3564 or click here to schedule online
References
Doucette RC, Sharp HT, Alder SC. Challenging generally accepted contraindications to vaginal hysterectomy. Am J Obstet Gynecol 2001;184:1386–9; discussion 1390–1. [PubMed]
Kluivers KB, Hendriks JCM, Mol BWJ, Bongers MY, Bremer GL, de Vet HCW, Vierhout ME, Brolmann HAM (2007) Quality of life and surgical outcome after total laparoscopic hysterectomy versus total abdominal hysterectomy for benign disease: a randomized controlled trial. J Minim Invasive Gynecol 14:145–152.
Stewart, K.I.; Fader, A.N. New Developments in Minimally Invasive Gynecologic Oncology Surgery. Clin. Obstet. Gynecol. 2017, 60, 330–348. DOI: 10.1097/GRF.0000000000000286